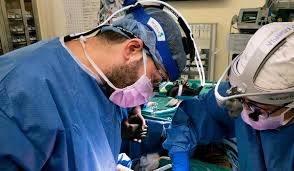
Disparities in care and outcomes are common, complex problems and are well illustrated by heart failure, from the initial diagnosis to the treatment of advanced disease.
Thank you for reading this post, don't forget to subscribe!In the US, Black individuals develop heart failure at a much younger age than individuals of other races, and the incidence for Black individuals is 50% higher than that for White individuals.1
Although the age-adjusted hospitalization rate for Black patients with heart failure in the US has decreased over the past 20 years, it was still approximately 2.2 times the rate for White patients in 2018.2 There is also a concern for disparities in unrecognized heart failure among Black patients and among female patients, as they are more likely to be diagnosed in the acute care setting despite having symptoms for months before diagnosis.3 The increased risk extends to those with end-stage heart failure, with Black patients accounting for 26.5% of hospitalizations coded as end-stage heart failure (2017-2020),4 which is double their 12.1% share of the overall US population in the 2020 US census.
The optimal treatment of end-stage heart failure is heart transplant, and the first step is to be placed on the transplant waiting list. In 1987, only 7% of those listed for transplant were self-identified as Black, but this number rose to 25% in 2019.5 Once listed, priority status is assigned based on standard criteria, although listing priority can be changed if the transplant team requests and is granted an exception.6
Despite the high cost and limited number of available donor organs, the total number of heart transplants has continued to improve for all groups, with 26% of heart transplants occurring in Black patients in 2019, up from 5% of all heart transplants in 1987.5 However, worrisome racial and ethnic differences persist. Among those listed from 2011 to 2020, Asian patients had the greatest probability of receiving a transplant (adjusted hazard ratio [AHR], 1.38; 95% CI, 1.28-1.48) followed by Hispanic patients (AHR, 1.04; 95% CI, 0.99-1.09) and then Black patients (AHR, 0.87; 95% CI, 0.84-0.90), all compared with White patients.7 The difference in transplant rate between Black and White patients appears to be decreasing over time.5
Moreover, there is evidence of fewer heart transplant listings for female patients. From 2011 to 2021, the percentage of wait-listed female patients decreased from 26% to 24%,8 while the percentage of hospitalizations coded for end-stage heart failure in women was 29% (2017-2020).3 Concomitantly (2011-2021), the percentage of transplant recipients who were female decreased from 28% to 26%.8 Overall, however, women have a higher rate of transplant, with 120 transplants per 100 patient-years on the waiting list compared with 100 transplants per 100 patient-years for men.8
To understand why differences exist in transplant rates for wait-listed patients, it is important to understand the complex process of offering donor organs. In 2018, the US donor heart allocation system was revised with the goals of making organs more widely available and with preference for the sickest patients. As intended, the change was followed by a significant increase in the number of hearts transplanted.8 The Organ Procurement and Transplantation Network offers a donor heart to an individual patient based on priority status (6 levels), distance, and blood type match. There are 68 permutations (classifications) of these 3 variables, ranked from status 1, with a primary blood type match within 500 miles, to status 6, with a secondary blood type match somewhere in the nation. What may be surprising to many is that most organ offers are refused by the transplant teams, and 44% of offered organs are never transplanted despite multiple offers.9 In the majority (67%) of declinations, the organ is felt to be poor quality. For others, the organ may be a poor match for the patient (the donor heart may be too large or too small for the patient), or patients may have had a change in clinical status that no longer makes them suitable for transplant.
Could the process of offering organs contribute to race- and sex-based differences in heart transplant rates? In this issue of JAMA, Breathett and colleagues10 provide insight into the process of offering organs following the US donor heart allocation policy change. They compared the number of organ offers to acceptance by race and sex and found that incidence of offer acceptance was higher for women than for men and for White patients than for Black patients. The median number of offers was 11 for Black men, 7 for Black women, 9 for White men, and 5 for White women. These differences persisted after adjustment for donor characteristics (age, left ventricular ejection fraction, history of cancer, distance from donor to candidate hospital, and difference in donor-candidate predicted heart mass). For transplant candidates, the authors controlled for presence of a ventricular assist device and order in which the organ was offered, which reflects severity of illness. Unfortunately, limited clinical data were available to the investigators that would have been available to those making the decision to accept an offer.
The study raises important questions. Do the data reflect an unconscious bias against Black patients and male patients by transplant teams? Are the groups different in important ways that were not measured and that would justify the organ declinations? The authors conducted sensitivity analyses for the patients with data on panel reactive antibody (a measure of allosensitization) but did not control for body mass index and blood type, which have been shown to be independently related to donor heart offer acceptance.
Of note, an analysis of the older allocation system did not find a significant difference in organ offer acceptance for Black patients.9 That study found wide variability in donor heart acceptance practices across centers, which suggests a potential for bias. Other studies have found that Black patients are clustered within centers, and it is possible that center-specific organ acceptance practices may have contributed to the observed racial differences.11
Is it possible that the new allocation system, which prioritizes patients receiving intensive, high-cost treatments, such as temporary mechanical circulatory support, has unintended consequences for equity? A recent study suggested that socioeconomic status has a stronger association with posttransplant outcomes after implementation of the new allocation system.12 While socioeconomic status was not a significant predictor of transplant or death or delisting while on the waiting list in the old system, low socioeconomic status was a predictor of poor waiting list and posttransplant outcomes in the new system. Given that half of Black patients on the waiting list were in the lowest third of socioeconomic status, they were more impacted than were White patients by the allocation change. This apparent change in impact of socioeconomic status is disheartening, since a study before the new allocation system indicated that socioeconomic status was becoming less important over time.13 Of note, the Organ Procurement and Transplantation Network reports on equity in its public dashboard,14 and this measure suggests continued recent improvement in equity overall by race and ethnicity but worsening sex-based equity (Figure). While this improvement for racial equity overall is encouraging, it does not rule out equity problems for specific racial and ethnic groups.
Figure. Trends in Race and Gender Equity in Time to Heart Transplant
Data are from Organ Procurement and Transplant Network equity dashboard14 and show the 12-month running average. The Access to Transplant Score indicates the likelihood of a patient on the waiting list receiving a transplant using various individual and community-level factors. A lower SD of the Access to Transplant Score for a characteristic indicates more equity for those grouped by the characteristic.
If the racial and sex-based differences in donor heart acceptance reflect clinically justified judgment on the part of the transplant team, this may be demonstrated in lower posttransplant mortality rates. However, prior work has found that greater selectivity was not associated with lower mortality.9 Mortality following transplant for Black recipients has historically been worse than mortality for White recipients. The difference varies with age, with the youngest adult patients (age, 18-30 years) showing a persistent mortality difference by Black and White race that was most pronounced during the first year after transplant.15
While socioeconomic status explains some of the past race-based disparities in mortality after heart transplant, it does not fully explain the differences. Other work has suggested the contribution of differences in immune function.16 Black patients have had significantly higher rates of acute rejection (13% vs 10% for White patients and 10% for patients from racial groups other than Black or White)5 and have higher levels of panel reactive antibodies and other measures of immune activation.16
The new heart transplant allocation system has successfully increased transplant access, but the effect on equity is less clear. Breathett and colleagues10 have identified a concerning but poorly understood difference in race- and sex-based transplant practice: organ offer acceptance. While the registry data used in these analyses have been crucial for exposing disparities, it is time to fund more detailed analyses of these practices, including in-depth studies of social determinants of health and race-based differences in immune responses in the setting of organ transplantation.
Paul A. Heidenreich, MD, MS, Department of Medicine, Stanford University School of Medicine